
More than 1.7 million people in the U.S. are diagnosed with sepsis each year1. 350,000 adults die from sepsis every year in the U.S. which represents more deaths than opioid overdoses, breast cancer, and prostate cancer combined1. Southwest Medical Center (SWMC), an acute care hospital located in Liberal, KS, joined Compass HQIC in September 2020. As they assessed their priorities for the Compass HQIC Workplan, they identified Sepsis Bundle Compliance as a priority for improvement through their work with Compass HQIC.
Prior to beginning the improvement work, patients received care based on current sepsis guidelines, however often elements of the bundle were delayed in deployment or in some cases missed altogether. Though sepsis education was provided to staff and clinicians in the past, newer staff did not have the benefit from prior sepsis education, resulting in knowledge deficits around best practices and sepsis guidelines. When the team analyzed gaps in processes, they identified a lack of urgency in sepsis response times. Overall, the team lacked momentum in improving sepsis bundle compliance rates as it had not been considered a priority focus for improvement efforts prior to the project.

Photo: The Emergency Department (ED) physicians and team members, ED Manager, Lab Team, Envision (ED Staffing Service used at SWMC), Sepsis Coordinator and the Performance Improvement/Risk Management Department at SWMC were key stakeholders for this performance improvement project.
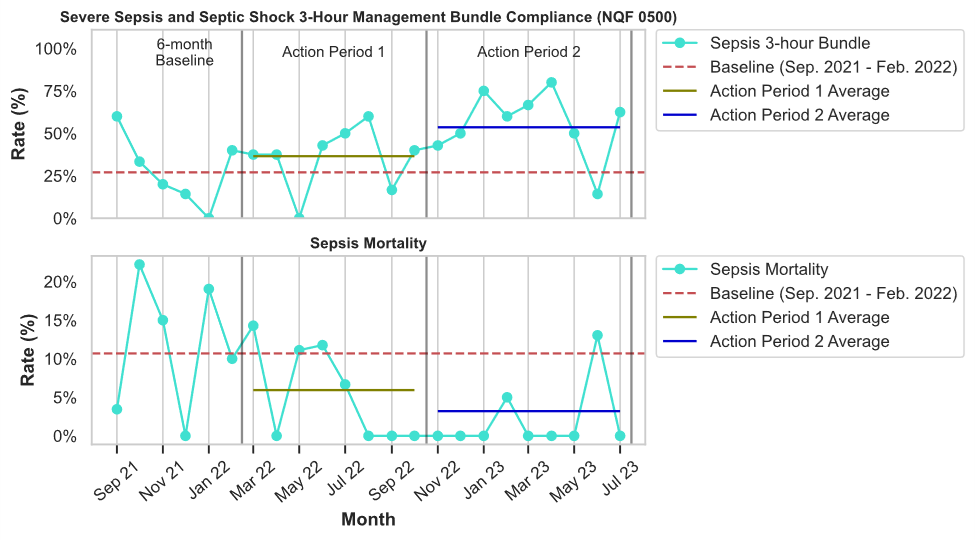
The quality improvement work began in earnest in March of 2022. At that time, the team set a goal of increasing knowledge and understanding of sepsis care, as well as increasing performance on the Sepsis Bundle Compliance Measure from 27% for the baseline period ending February 2022 to an average of 57% bundle compliance by the end of the project period.
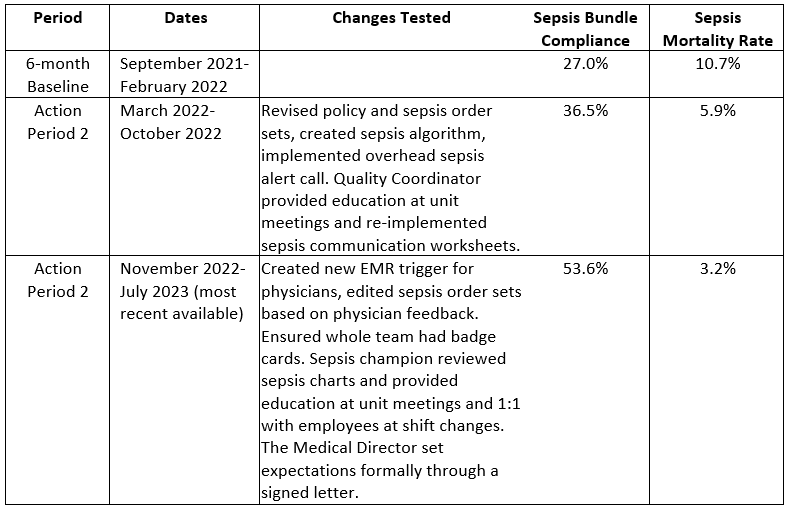
The team began their implementation process in March 2022, by revising the sepsis policies, procedures, and order sets, creating a sepsis algorithm, and implementing an overhead sepsis alert call. The Quality Coordinator, Jandi Head, RN, provided education at ED unit meetings and re-implemented the sepsis communication worksheets. They set a go-live date for the new policies and procedures for April 2022. Unfortunately, the initial change deployment was not successful due to the initial lack of staff buy-in, post-pandemic burnout and lack of interest in the changes being tested.
Jandi says the project initially felt rushed and should have included more staff input in the initial stages to foster staff support and eventual buy-in for change implementation. After the initial failed implementation period, the team revisited barriers and monitored sepsis data to determine the reason for the initial project failure. The team met to discuss implementing another action plan in November 2022. They looked at how their electronic health record (EHR) triggers a sepsis alert and created an alert for the physicians and again revised the sepsis order sets based on new physician feedback.
They also ensured the whole ED team had sepsis badge cards. Their custom badge cards were adapted from a sample provided by Wesley Medical Center and provide sepsis criteria, vital signs, laboratory ranges, sepsis care measures and sepsis guidelines.
The SWMC team created a report that would identify patients that met sepsis criteria and Sepsis Champion, Katie Hayes, RN reviewed the identified charts to provide prompt feedback to the team. The team provided education on the latest changes to policies and procedures during the ED unit meetings, 1:1 with employees at shift changes. An official letter was sent to all the physicians from the Medical Director, listing expectations regarding the new sepsis procedures.
When treating sepsis, time is of the essence, though SWMC initially struggled to create a culture of sufficient urgency in response to sepsis. It was a challenge to motivate staff to respond to sepsis with the same sense of urgency as stroke or myocardial infarction. SWMC worked to change sepsis engagement by sharing stories about SWMC patients, both positive and those with opportunity for improvement. They asked team members to imagine the patient as a loved one and provide the care they would want for someone they loved.
To facilitate rapid response and initiation of testing and treatment protocols for patients exhibiting signs and symptoms of sepsis, the team implemented revised sepsis standing orders to facilitate nurses entering the sepsis standing orders. This new change in workflow was met with resistance, so SWMC set the expectation that when a nurse alerted a physician of a suspected sepsis patient, the physician was expected to see the patient and place orders within five minutes of the alert, otherwise nursing staff would enter the orders according to SWMC standing order protocols for sepsis.
SWMC provided sepsis communication worksheets in every room and posted the sepsis treatment algorithm in each room to keep the treatment algorithm at the forefront of the care team’s minds when treating patients. Additionally, SWMC set an initial expectation that staff were to complete a sepsis communication worksheet on every patient to aid the team in thinking about the sepsis with every patient.
Much has changed at SWMC since the start of this improvement project. Throughout the process, when barriers to success were identified, the team responded by investigating and acting to address the barriers. In some cases that identified opportunities for workflow revision, re-education, or identification of systems issues. The hospital currently strives for a 24-to-72-hour chart review response time for patients treated for sepsis which allows the team to closely monitor trends in addition to individual patient care.
Today, Emergency Department staffing trends contribute to the project success. More physicians have chosen SWMC as their primary work site or have set a regular work schedule at the hospital as compared to the beginning of the project when physicians were sometimes unfamiliar with the SWMC sepsis routine and expectations.
Though SWMC has seen marked improvement since the beginning of the project, the work is not complete. The team hopes to meet their goal of 57% Sepsis Bundle Compliance by the end of 2023 but still have work to do. Documentation often lacks the appropriate clinical rationale for not ordering fluid resuscitation as well as the requirements around repeat volume status. They plan to utilize the EHR to reduce the burden associated documentation requirements. Jandi is developing a one-page guidance around fluid resuscitation to post in the physician areas.
Though the changes were initially met with some resistance and lack of engagement, with time, communication and sepsis education, team members demonstrate a greater understanding of the sepsis routine and workflows required to meet the facility’s expectations. For SWMC, sepsis improvement is ongoing. The team won’t consider themselves successful with the project until sepsis care measures become as second nature as obtaining an EKG for a patient who reports chest pain.
1 Sepsis Alliance: 2023 Sepsis Awareness Month Toolkit https://www.sepsis.org/wp-content/uploads/2023/06/2023-Sepsis-Awareness-Month-Toolkit.pdf
